5-4-5 Hormones and Co-Existing Conditions in Type 1 Diabetes
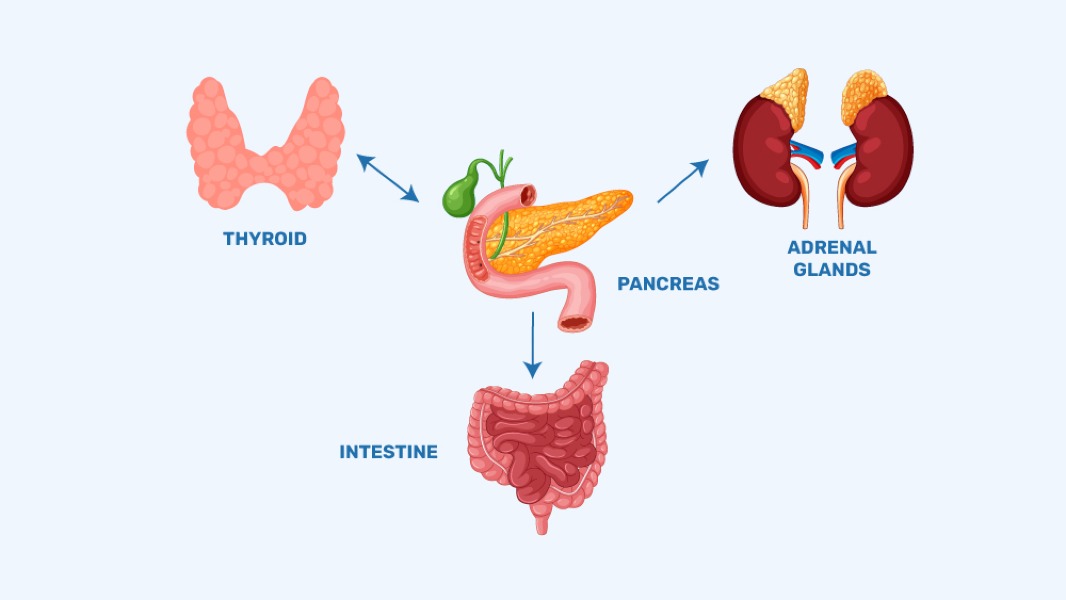
How thyroid, adrenal, and coeliac conditions affect blood glucose and performance
People with type 1 diabetes have a higher risk of developing other autoimmune conditions, including thyroid disease, Addison’s disease, and coeliac disease. These conditions can significantly influence insulin sensitivity, carbohydrate absorption, and blood glucose patterns. Understanding early warning signs and appropriate management strategies helps support stable glucose control, physical performance, and long-term health.
Why Co-Existing Conditions Matter in Type 1 Diabetes
Autoimmune conditions often occur together. Around one in five children and adolescents with type 1 diabetes have thyroid antibodies, approximately 8% develop coeliac disease, and a small percentage develop adrenal insufficiency (Addison’s disease). These conditions are more common in females.
Each condition affects blood glucose differently:
- Some increase insulin resistance and cause hyperglycaemia
- Others increase insulin sensitivity and raise hypoglycaemia risk
- Some interfere with nutrient absorption and digestion
As a result, unexplained glucose instability may sometimes be related to an underlying co-existing condition rather than insulin dosing alone.
Early recognition supports timely treatment and improved metabolic stability.
How Autoimmune Conditions Affect Blood Glucose
Different conditions influence glucose regulation in specific ways:
- Thyroid disorders affect metabolism and insulin needs
- Adrenal insufficiency alters cortisol levels and glucose release
- Coeliac disease disrupts carbohydrate absorption
Monitoring symptoms alongside CGM data helps identify potential problems early.
Common Co-Existing Conditions and Management
Hashimoto’s Thyroiditis (Hypothyroidism)
Typical signs:
- Frequent hypoglycaemia
- Weight gain
- Fatigue
- Cold intolerance
Management:
- Levothyroxine replacement therapy
- Temporary reduction in basal insulin may be needed during treatment initiation
- Regular thyroid function monitoring
Graves’ Disease (Hyperthyroidism)
Typical signs:
- Persistent hyperglycaemia
- Heat intolerance
- Palpitations
- Eye symptoms
Risks:
- Increased risk of diabetic ketoacidosis if untreated
Management:
- Antithyroid medication
- Possible temporary basal insulin increase
- Adequate hydration
- Frequent glucose monitoring
Addison’s Disease (Adrenal Insufficiency)
Typical signs:
- Recurrent unexplained hypoglycaemia
- Salt craving
- Severe fatigue
- Low blood pressure
Management:
- Daily hydrocortisone replacement
- Higher post-meal insulin doses may be required
- Stress-dose steroids during illness or competition
- Carry fast-acting carbohydrates at all times
Coeliac Disease
Typical signs:
- Iron-deficiency anaemia
- Abdominal discomfort
- Bloating
- Poor growth in children
- Weight changes
Screening:
- IgA tissue transglutaminase antibodies at diagnosis
- Repeat after 1 year, then every 3 years or if symptomatic
Management:
- Strict gluten-free diet
- Monitoring of post-meal glucose due to higher glycaemic index of some gluten-free foods
- Possible adjustment of prandial insulin doses

Quick Screening Checklist
Regular screening supports early diagnosis:
- Annual TSH and thyroid antibodies
- Morning cortisol if fatigue and frequent lows occur
- Coeliac serology every 3 years or if symptoms appear
Discuss screening results regularly with your healthcare team.
Training and Performance Tips
- Record glucose changes when starting or stopping thyroid or steroid medication
- Increase hydration during hyperthyroid phases
- Monitor digestion and glucose after changing to a gluten-free diet
- Inform coaches about adrenal insufficiency and emergency steroid needs
- Review insulin settings after major treatment changes
- These steps support safer training and reduce unexpected glucose fluctuations.
Long-Term Management and Confidence
Managing co-existing conditions alongside type 1 diabetes requires teamwork between the individual, endocrinologist, and primary care providers. With structured screening, appropriate treatment, and flexible insulin adjustments, most people can maintain stable glucose control and continue participating fully in sport.
Understanding these conditions improves long-term health, safety, and performance.
Related Articles

5-4-3 Menstrual Cycle, Sport, and Blood Glucose in Type 1 Diabetes
How hormonal changes influence insulin needs, training, and glucose control

2-3-1 What is Hypo and How to Manage It?
Recognising low blood sugar and staying safe during physical activity

2-4-1 What is Hyper and How to Manage It?
Understanding high blood sugar and staying safe during physical activity

5-4-2 Beyond Insulin: How Hormones Shape Blood Glucose in Type 1 Diabetes
Understanding hormonal changes that affect glucose control during sport and daily life

4-1-3 Starting or Returning to Sport with Diabetes: Talking to Your Healthcare Professional
How to prepare for a safe and personalised exercise plan